
‘Palliative care’.
I’d heard the term before. I knew it had something to do with end of life care, but I had to Google it to see if it meant something else. Something more positive.
It didn’t.
That was the phrase said by a doctor the day after I’d been diagnosed with bowel cancer, back in 2017, aged 46.
Palliative treatment would mean they weren’t trying to cure my cancer, but just trying to alleviate my symptoms to keep me comfortable until I died.
I was petrified.
I’d been feeling ill for about 18 months and had been trying to move things along with my GP for about a year, but was just presuming and hoping that I’d be OK.
That maybe I was making a fuss about nothing – so I didn’t push.
I’ve had bowel issues and IBS since my teens, so I thought that my usual symptoms – alternating diarrhoea and constipation, bloating, stomach aches – were just getting worse with age, stress, and perimenopause.

Initially, my GP ran blood tests and noticed my inflammatory markers were high. I was prescribed antibiotics and my symptoms eased, and my GP didn’t seem too worried about it, so I didn’t follow up.
But by January 2017, my symptoms got worse. I constantly felt like I wanted to go to the toilet, but nothing would happen.
I had pains in my lower belly and sometimes a slight pinkness on the toilet paper.
After several GP appointments, I was referred to a gastro-intestinal consultant. But while waiting for my first scan that September, my health plummeted.
Food was causing so much digestive pain and upset that I couldn’t eat. I dropped three stone in eight months.
At this point, I was suffering from stomach pains, vomiting, and unable to produce any bowel movements.
I went to get a private consultation appointment for my scan, as the original one was booked for November, and I couldn’t wait any longer.

Finally, two days after the scan, I got the call. Doctors told me to pack a bag and get to the hospital immediately.
My husband, and I decided that my mum should drive me to hospital. My husband would stay to greet our two daughters from school, then 10 and 12, to explain what was happening. To say that mummy hadn’t been feeling very well and had gone into hospital to get better.
In hospital, I was told there was a blockage in my colon and I needed a colonoscopy. It was a tumour.
The next day, I was told that I had bowel cancer – and that treatment might be palliative only.
I couldn’t stop thinking about my two girls: how was I going to break this news to them?
Thankfully, doctors agreed they could operate and I was booked in for surgery five days later – but I was told it was to be ‘aggressive’.
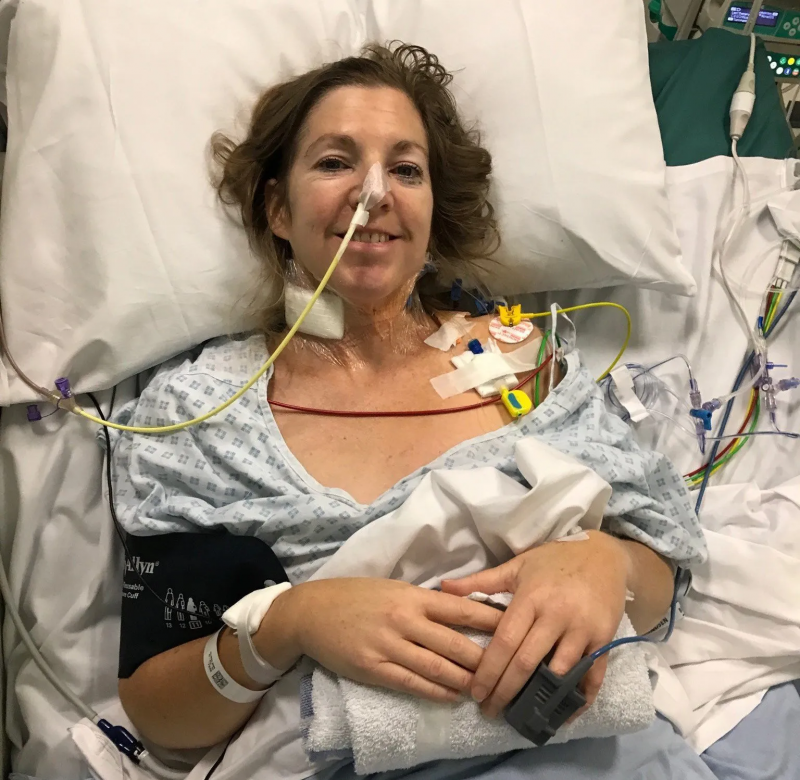

Doctors explained that my lower sigmoid colon was to be removed, along with some of my upper intestine, my bladder, ovaries, cervix and uterus. I would be given stomas to replace my missing colon and my bladder (a urostomy).
It was a horrendous shock and I remember thinking that people didn’t survive this. This surgery did, however, save my life.
After a month in hospital, I was delighted to go home before I started six months of chemotherapy.
I took comfort in talking about what had happened. It was emotional, but cathartic – and after seeing lots of friends and family, it became easier.
I wanted to put it behind me, but knowing I still had to have chemo, I decided to work on building up my strength.
In the first week, I just wanted to get to the end of the road. But I walked a little more each day, and got gradually stronger so I could go on longer, faster walks.
Chemo made me feel tired and sick, but generally I was able to do most things I wanted to do.

Walking got me out of the house, into the fresh air. I was doing something I enjoyed, and I liked feeling that I was getting well and strong again.
In June 2018, after my chemo ended, I did a 50km charity walk along the Cotswold Way for Bowel Cancer UK. I loved it and it gave me a sense of normality.
By now, I was feeling a lot stronger and fitter. So, that summer, I started trying to do a little bit of jogging when I was out walking.
Quite quickly I was able to get back into doing 5km runs, working up to 10km runs – stopping whenever I felt sore. After a year or two, I was able to start training to do a half marathon, which I’d never done before I was ill.
I found that one of the most daunting aspects of my journey was adjusting to life with stomas.
The biggest impact is that you don’t use the toilet anymore, instead you poop into a bag that is attached to the stoma (or opening) on your belly, and you have no control over when this happens.

The bag for the bladder stoma (urostomy) has a little tap on it so you can empty it into a toilet throughout the day.
Initially, I felt awkward and embarrassed to be out with my stomas. I was worried that other people might see, hear or smell them.
It took time to build up my confidence, but support from understanding friends eased the process.
By now, I thought it was all over – and I adjusted to my new normal. Except, in 2020, I learned that the cancer had returned.
That February, I had my annual check-up, and got the results in late March. My consultant told me that a lesion on my left lung had morphed into cancer.
It felt like everything was going wrong, and it was made worse knowing that the NHS was struggling with the pressures of Covid.
That July, after being diagnosed with the return of bowel cancer (now stage 4), I had half my left lung removed.
Then cancer was found in my right lung, and in my lymph nodes. I felt bereft, I’d already been through so much.
But it got worse.
That November, as I started chemo, I was told that I might only have 18 months to two years to live. Once again, I was told that treatment was palliative, not curative.
I felt low, but I pushed through treatment. I was determined to make my lifestyle as healthy as possible.
I kept running, cut out alcohol and became even more mindful of my diet. I found that fresh air and exercise really helped counteract the effects of chemo.

And my treatment and healthy lifestyle seem to be working.
Amazingly, three years of bi-weekly chemotherapy later, things are currently stable.
I stopped chemo in November 2023 and two scans since have shown no new cancer. I can stay off chemotherapy treatment as long as my scans stay the same.
With changing my lifestyle, I feel like I’ve helped my body fight the cancer alongside the chemo.
The last seven years have been a journey, but I’ve learnt to celebrate the small wins – despite the ever-present worry lurking in the back of my mind: what if the next scan shows a recurrence?
Most of the time though, I feel positive and try to focus on the future.
I urge you not to ignore any pain, or symptoms and to go to the doctor if there’s anything you’re worried about. To push for help.
I sometimes wonder where I’d be if I had acted earlier – maybe we could have caught the cancer sooner, but I can’t live like that. I have to be positive.
Having cancer has forced me to understand the importance of looking after myself and to evaluate what is most important to me – being with loved ones, and enjoying walking and running in the countryside.
More from Metro
-

Run clubs have become our new nightclubs – here’s why
I’m feeling cautiously optimistic.
Do you have a story you’d like to share? Get in touch by emailing jess.austin@metro.co.uk.
Share your views in the comments below.
Sign up to our guide to what’s on in London, trusted reviews, brilliant offers and competitions. London’s best bits in your inbox
Disclaimer: The copyright of this article belongs to the original author. Reposting this article is solely for the purpose of information dissemination and does not constitute any investment advice. If there is any infringement, please contact us immediately. We will make corrections or deletions as necessary. Thank you.





